Page 5 - Valley Life & Health
P. 5
THE MORNING CALL SATURDAY, MAY 25, 2019 5
Because GERD exists in four different stages, without damage to the rest of the esophagus. “It
it is important for doctors to diagnose exactly is a microwave kind of energy, and we take the
what stage the patient is in so that they know scope and burn out the Barrett’s tissue. You don’t
what the best treatment option will be. just do the treatment on anyone, however. There is
In Stage 1, the patient has only minor damage selection criteria,” warns Dr. Mittal. To receive RFA,
in the esophagus, and medication combined a patient would have to have advanced Barrett’s,
with lifestyle changes usually helps manage their as well as risk factors such as being overweight,
symptoms. In Stage 2, there is an increase in smoking or drinking alcohol excessively.
the severity of their symptoms and they should Mittal says that about 95 percent of patients
consider seeking out a gastroenterologist to help 1 that receive RFA can go back to work or resume
them manage their symptoms. In Stage 3, there is normal activity within a day or two, and must stick
a noticeable decrease in the patient’s quality of life, When the reflux barrier becomes weak or lax, stomach to a liquid diet for at least one day.
and their symptoms can no longer be addressed acid comes back up into the food pipe, causing GERD. For some GERD sufferers, valve repair may
with PPIs. In Stage 4, there is noticeable change to be the only way to provide them the relief that
the affected tissue in the esophagus, which is most medications do not. For a long time, an invasive
likely in patients with years of repeated damage or procedure called Nissen fundoplication – where
patients who took too long to see a doctor. doctors make an incision and then wrap the top of
“We have established that the acid that comes the stomach around the esophagus to recreate a
back up into the esophagus causes chemical burn. valve – was the only option. Now, a less invasive,
Over time, that can transform into something called non-surgical procedure called transoral incisionless
®
Barrett’s esophagus. Barrett’s means the lining of fundoplication, or TIF , is being performed – with
2 an extremely high success rate – by Amit Sohagia,
MD, gastroenterologist with Easton Hospital.
The procedure, which takes about 45
A camera called an endoscope is inserted into esophagus
and provides direct visualization for the TIF® procedure. minutes to one hour under general anesthesia,
reconstructs the anti-reflux barrier between the
stomach and esophagus by going through the
mouth rather than through an abdominal incision.
Amit Sohagia, MD, “TIF was approved by the FDA in 2007 and
®
gastroenterologist we started performing the procedure [at Easton
with Easton Hospital. Hospital] in 2016. Since then, we’ve treated around
130 patients with excellent results. There is no
Photo courtesy of complication in a majority of the patients, and we’ve
Easton Hospital
3 seen a 70 percent success in terms of patients who
are still off their medications,” says Dr. Sohagia.
the esophagus changes over time from acid burn “Even if they have to take medication, their reflux
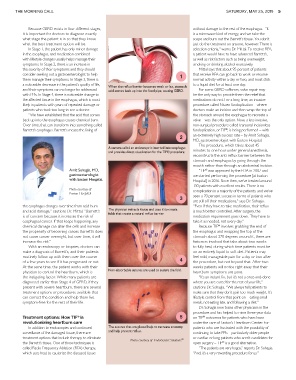
and acid damage,” cautions Dr. Mittal. “Barrett’s The physician retracts tissue and uses it to create is much better controlled. After surgery, the
folds that create a natural reflux barrier.
is of concern because it increases the risk of medication requirement goes down. They have to
esophageal cancer. If that keeps happening, any take it as needed, not every day.”
chemical damage can alter the cells and increase Because TIF involves grabbing the end of
®
the propensity of becoming cancer. Barrett’s does the esophagus and wrapping the top of the
not cause cancer overnight, but over time, it will stomach about 270 degrees around it, there are
increase the risk.” fasteners involved that take about two weeks
With an endoscopy or biopsies, doctors can to fully heal, during which time patients must be
make a diagnosis of Barrett’s, and their patients on an entirely liquid to soft diet. Patients may
routinely follow up with them over the course feel mild, manageable pain for a day or two after
of a few years to see if it has progressed or not. 4 the procedure, but not beyond that. After two
At the same time, the patient works with their weeks patients will notice right away that their
physician to control the heartburn, which is Non-absorbable sutures are used to secure the fold. heartburn symptoms are gone.
the instigating factor. While many patients are “It’s an instant fix, but it’s not a once-and-done
diagnosed earlier than Stage 4 of GERD, if they where you are cured for the rest of your life,”
present with severe heartburn, there are several cautions Dr. Sohagia. “We always tell patients to
treatment options or procedures available that make sure that they don’t gain too much weight. It’s
can correct the condition and help them live lifestyle control from that point on – eating small
symptom-free for the rest of their life. meals, not eating late, and following a diet.”
Dr. Sohagia now trains other physicians in the
procedure and has helped to mine three-year data
Treatment options: How TIF is 5 on TIF outcomes for patients who have been
®
®
revolutionizing heartburn care under the care of Easton’s Heartburn Center. For
In addition to endoscopies and continued The sutures that are placed help to recreate anatomy patients who are frustrated with the possibility of
surveillance of the damaged tissue, there are and help prevent reflux. continuing to take PPIs – particularly older people
treatment options that include therapy to eliminate Photo courtesy of EndoGastric Solutions ® or cardiac or lung patients who aren’t candidates for
®
the Barrett’s tissue. One of those techniques is open surgery – TIF is a good alternative.
called Radio Frequency Ablation (RFA) therapy, “The patients are very happy,” reports Dr. Sohagia.
which uses heat to cauterize the diseased tissue “And, it’s a very rewarding procedure for us.”